At Carnegie Mellon University, breakthroughs in robotics, materials science and bioengineering are increasingly shaped by a shared goal — making health care more precise and less burdensome for patients and providers. Meet four CMU-affiliated startups that are translating academic research into tools that could improve health care for millions of Americans.
Turning robotics research into data-driven prosthetic care
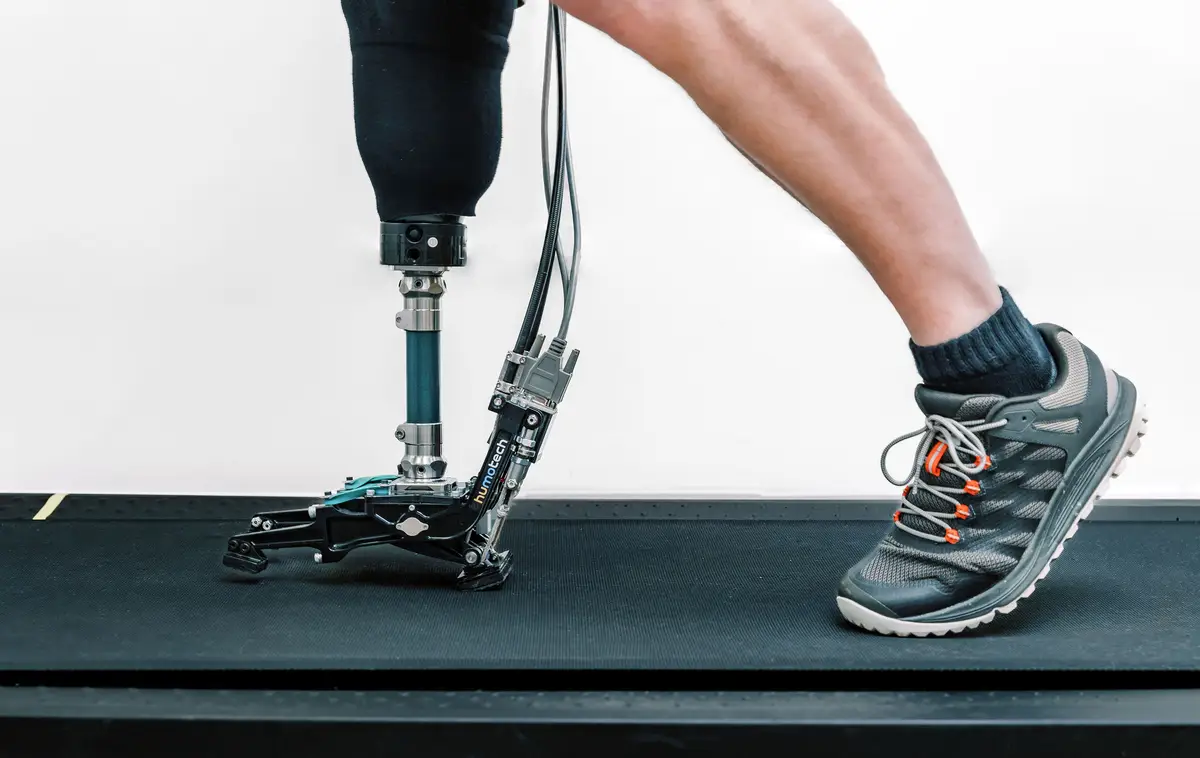
For people who need a prosthetic limb, the options are hard to navigate, with cost and functionality varying widely. CMU alumnus Josh Caputo built Humotech(opens in new window) to change that. The company creates wearable robotic systems that allow researchers and clinicians to test, personalize and improve prosthetics that are right for the people who need them.
Caputo said Humotech is translating years of robotics research into clinical care. Its prosthetic foot-selection system lets people with limb loss try different options in real time — measuring gait, balance and comfort while capturing patient feedback, much like a test drive for a car.
“Patients are usually handed one device and told, ‘This is it,’” Caputo said. “We want to put patients in the driver’s seat and make the process more data-driven and human-centered.”
Caputo’s path to entrepreneurship began at Carnegie Mellon, where his Ph.D. research in Mechanical Engineering(opens in new window) focused on the design and control of robotic prosthetic feet. What started as an effort to design better devices evolved into a deeper realization. The real challenge wasn’t inventing a single perfect prosthetic, but helping people choose what works best for their bodies and lives.
“This is the kind of invention that could only come out of CMU,” he said, pointing to the university’s blend of robotics, design thinking and close ties to clinical partners in Pittsburgh.
A first-of-its-kind implant system could change how chronic GI diseases are treated
For patients with chronic gastrointestinal diseases like Crohn’s disease, treatment often includes daily medications. Edulis Therapeutics(opens in new window), is working on a different approach. They created a tiny implant that continuously delivers medicine to patients over the course of a year, then dissolves.
About the size of a grain of rice, the implant could be placed in patients during a routine endoscopic procedure, said CMU alumnus Spencer Matonis, the company’s founder.
“The idea is to give physicians a new tool. Instead of relying on systemic drugs that circulate throughout the whole body, we can deliver existing medications more effectively by putting them right where they’re needed,” he explained.
Matonis worked alongside two practicing gastroenterologists to design the device, which he said represents a first-of-its-kind therapeutic intervention for Crohn’s disease. The technology is designed as a platform, meaning it could eventually be adapted for use with multiple medications for diseases like ulcerative colitis and other conditions.
Edulis is still in the preclinical stage, but the company has already completed four proof-of-concept studies in animal models. They are currently seeking investors to support their next phase of development to work toward clinical trials in humans.
For Matonis, the goal is to transform how chronic GI diseases are treated by making therapies more precise, more durable and easier for patients to live with.
“If we can give patients a year of sustained treatment from a single, minimally invasive procedure,” he said, “that could be a major shift in how these diseases are managed.”
Building living tissue for diabetes treatment
Another CMU-affiliated startup, FluidForm Bio(opens in new window), is taking a unique approach to treating disease: building living human tissue.
A spinout from the lab of CMU professor Adam Feinberg(opens in new window), FluidForm Bio is based on advances in 3D bioprinting that allow researchers to create complex biological structures using materials found naturally in the body, like collagen. The company’s technology prints cells and proteins inside a supportive gel, enabling far more precise and biologically realistic tissue structures than traditional methods.
FluidForm Bio’s primary focus is treating Type 1 diabetes by creating pancreatic-like tissue designed to restore the organ’s insulin production. Rather than managing symptoms, the approach is designed to help people regain abilities they’ve lost to disease.
The technology has already been tested in mouse models, and the company is raising funds to support large-animal studies, the final step before clinical trials.
“This is really about making human tissue that can work in the body,” Feinberg said. “Once we realized we could reliably print collagen — the body’s main structural protein — it opened the door to therapies that weren’t previously realistic.”
Beyond diabetes, FluidForm Bio is also part of a federally funded ARPA-H project(opens in new window) to build functional human liver tissue. The goal is to create temporary liver support for patients with acute liver failure, allowing their own organs time to regenerate and potentially reducing the need for transplants.
“If this works the way we believe it can,” Feinberg said, “it could fundamentally change how we think about treating disease — not with drugs alone, but with living tissue.”
Helping surgeons see what they can’t feel
In many surgical procedures, even experienced clinicians must rely on subjective evaluation and what they can infer rather than quantitative data, a gap Advanced Optronics(opens in new window) is working to close. The company makes sensor-enabled surgical tools to provide direct, objective feedback and enhance surgeon perception..
Take cochlear implants, small devices designed to restore the sense of hearing to patients.
“Cochlear implantation is an extremely delicate microsurgical procedure, but today, surgeons lack direct feedback once the device enters the inner ear,” alumnus Jay Reddy explained. “Advanced Optronics is about enhancing surgeon perception during minimally invasive procedures.”
The company grew out of Reddy’s research at Carnegie Mellon, where he began exploring how advanced microfabrication techniques could be applied to medical devices. The technology developed at Advanced Optronics is undergoing preclinical validation with surgeons, including early testing in Pittsburgh.
“Our goal isn’t to replace surgical skill,” Reddy said. “It’s to give surgeons better information at the moments when it matters most.”
By turning subtle physical signals into quantitative feedback, Advanced Optronics is helping to make complex procedures more consistent and predictable, an approach that reflects a broader shift across CMU-rooted health startups toward precision tools that support both patients and providers.
Source link